Cesarean Birth
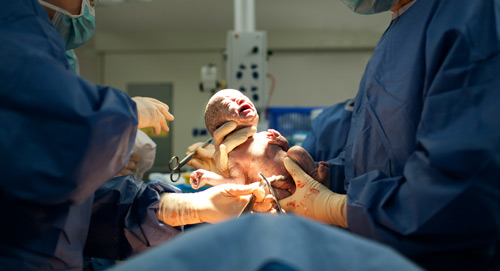
In the operating room, an incision is made through the abdomen and then into the uterus, and your baby is lifted-out. If you are awake, you can see your baby right away. The placenta is then pulled away from the uterine wall and delivered, and your incisions are repaired. While baby is born 5-10 minutes after surgery begins, the entire procedure takes about an hour.
Planned
- You've had delivery-complications or a cesarean birth before
- Your placenta is in the wrong position
- Baby is in breech (head-up instead of head-down)
- There is a "cord issue" (trouble with the umbilical cord being wrapped around baby's neck)
Unplanned
"Emergency" cesarean births may be performed because of your baby's health, size or position, or because of your own health. In most cases, you are prepared for surgery immediately after this decision is made, without much time to prepare yourself emotionally. You may also be unconscious during an emergency cesarean.
Vaginal Birth After Cesarean Birth (VBAC)
The American College of Obstetricians and Gynecologists (ACOG) states that most women with one previous cesarean birth - who have a low transverse incision in their uterus (ask your doctor or nurse-midwife about this) - are candidates for Vaginal Birth after Cesarean Birth (VBAC). It is also recommended that such women should be counseled by their doctor or nurse-midwife about VBAC, and offered the chance to try labor.
There may be special concerns for women who have had more than one cesarean birth, whether they attempt VBAC or a repeat cesarean. It is important to talk with your doctor or nurse-midwife about your feelings and concerns. We recommend talking with other women who have given birth vaginally after a cesarean birth, and including your partner in these discussions.
Cesarean Birth
To purchase the full video, please visit laughandlearn.com
After Surgery: What Happens Next?
After your baby is born you will be moved from the operating room to the recovery room for 1 to 2 hours, until the anesthesia wears off and you are stable.
Your doctor or nurse-midwife may press down on your belly several times after your baby's birth, to make certain that your uterus is returning to normal. This also helps you to pass blood clots from your uterus; a process that would happen naturally had you gone through labor. You may try using your relaxation or breathing techniques (from your birthing classes) if you experience discomfort here. You will still have the IV and the catheter from your surgery, and you'll also have a blood pressure-cuff, a finger clip (to measure your body's oxygen level), and possibly an oxygen mask.
About every 15-minutes, a nurse will check on you to assess the firmness of your uterus, the amount of vaginal bleeding, your pain relief needs (& how the anesthesia is wearing-off), the bandage on your incision and your vital signs.
Visitors are normally allowed during this time and - if he or she is doing well - your baby may be with you! (Check with your hospital policy & procedures about this.) Try to hold your baby, and try breastfeeding now if you plan to do so. When nurse feels that you are ready, you'll be moved to a room for the remainder of your hospital-stay.
If your baby is in a newborn intensive care unit or a special care nursery, you may be taken there to see your baby before you are settled into your postpartum room. Sometimes it becomes necessary to transfer your baby to another hospital for special care. If this is the case, take whatever opportunity you can to see and touch your baby before she is transported. You'll be kept informed of her progress. You may even be healthy enough to be discharged early to visit the other facility and see your baby.
Your catheter and IV will be removed as soon as you are drinking liquids and taking foods.
Getting Out of Bed
Approximately 8-hours after surgery, your nurse will help you get out of bed to walk around the room. The next day, you should be able to go to the bathroom and walk in the hallways. It may be hard at first, but walking is one of the most important things you can do to speed your recovery.
Ask the nurse to lower your bed as close to the floor as it goes. (If you are lying flat, roll onto your side and prop yourself up on one elbow. Then use both arms to push yourself up into a sitting position.) Next, gently scoot yourself toward the side of the bed and use your hands to lift your upper thighs - one at a time - over the edge. Dangle your legs over the side for a few moments. As you stand, support your incision with a pillow or your hands.
Walking & Standing
Many women stoop or lean forward in an attempt to protect their incision, but standing-up straight is best, as it naturally lifts the weight of your abdominal organs from your incision. If you are experiencing pain, it is always helpful to gently support your incision with a pillow. Creating a "supportive splint" by tightening your abdominal muscles when changing positions or standing, will encourage your muscles to heal, and reduce the pain overall.
Getting Back into Bed
Adjust the back of your bed into an upright position (as a nurse or your partner for help if needed). Support your incision with a pillow or your hand while lifting your legs - one at a time - back onto the bed.
Muscle Spasms
If you experience muscle spasms or painful contractions, it's because your abdominal muscles are attempting to protect themselves from further injury. Relaxing these muscles is very important for comfort.
Here are some things to try:
- Close your eyes and breathe gently, slowly, and deliberately into the painful area.
- Place your hands gently over the incision and focus your breathing into your hands, allowing the spasm to soften.
- Continue this for 15-minutes, or longer if necessary. Your discomfort should decrease.
 PREGNANCY
PREGNANCY  GIVING BIRTH
GIVING BIRTH  BABY CARE
BABY CARE  HEALTH & SAFETY
HEALTH & SAFETY  FUN STUFF
FUN STUFF  FAMILY
FAMILY 